The Low Glycemic Index Treatment (LGIT) was developed in 2002 by Dr. Elizabeth Thiele and dietitian Heidi Pfeifer at Massachusetts General Hospital. As an alternative to the Classic Ketogenic Diet, the LGIT places emphasis on the intake of complex carbohydrates over simple sugars, restricting both the total amount of daily carbohydrate and the type, based on what is known as the Glycemic Index (GI).
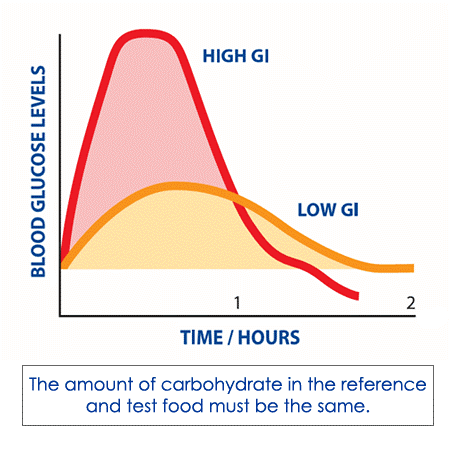
The GI of a food refers to the extent to which it raises blood sugar (glucose) levels after ingestion. Foods with a low GI (less than 50), are digested, absorbed, and metabolized slowly, resulting in small fluctuations in blood glucose and insulin levels, which has been shown to raise the seize threshold.
In addition to the GI, the metabolism of carbohydrates is slowed by foods eaten at the same time that contain fat or fiber, making meal composition distinctly important to the LGIT. Meals are based on portion sizes using household measurements, with a goal of no more than 60 grams of low glycemic index carbohydrates per day, balanced alongside sources of fat and protein.
Less rigidity allows the LGIT to be initiated on an outpatient basis, though consistent, long-term laboratory and medical surveillance is still required.
Think the Low Glycemic Index Treatment is right for you? Talk to your doctor and Registered Dietitian for a comprehensive evaluation.
