Taking its cues from the aviation industry, where pilots are expected to train for hundreds of simulated flight-hours, BMC has created in the Alan D. Solomont & Susan Lewis Solomont Clinical Simulation & Nursing Education Center a nexus for immersive experiential learning for every employee involved in patient care.
Using high-fidelity computer-assisted manikins in realistic patient care environments, from the operating room to the inpatient room, we can simulate virtually any clinical situation. We then gather the caregivers for that situation — from nurses and respiratory technicians to resident physicians and attending physicians — and run the scenario. This provides a unique, friendly, and safe environment in which to learn how to improve our delivery of patient care, and to make BMC the safest hospital possible for our patients.
About the Solomont Center
Our Space
Operating Room
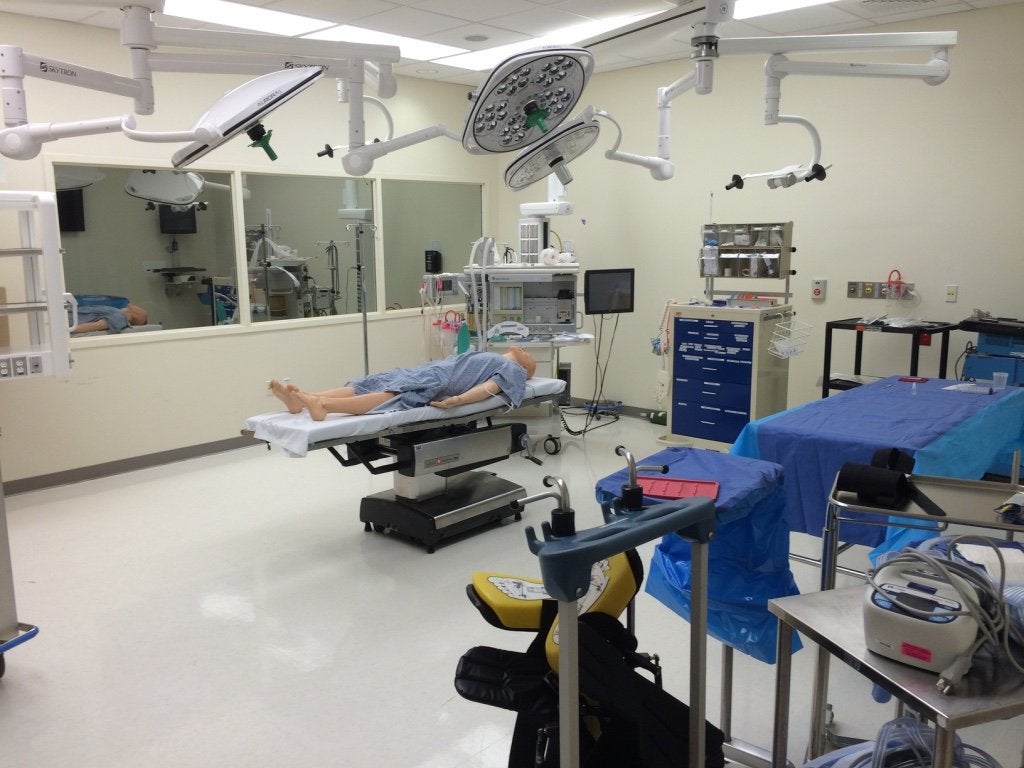
Our spacious operating room contains a SimMan 3G, airway cart, fully functional anesthesia setup, computer on wheels, OR table, table for OR instruments, gas connectors with running air and oxygen, wall phone, and 65-inch monitor with video/PowerPoint capabilities.
Task Room
Our multipurpose task room is home to several Storz laparoscopic technique trainers. The task room is open 24 hours to all residents who perform laparoscopic procedures.
HPS (Human Patient Simulation) Rooms
There are four inpatient rooms that can be set up for adult or pediatric situations. Each room contains a SimMan or SimBaby manikin, gas connectors with running oxygen and air, a wall phone, and a 32-inch monitor with video/PowerPoint capabilities.
Control Rooms
There are four control rooms, each adjacent to a human patient simulation room, in which the technical operator and clinical educator facilitate the simulation scenarios for the learners.
Conference Room
The Solomont Center conference room seats 10–12 learners and has videoconferencing capabilities.
Hallway
Our hallway space has audio/video recording capability to capture patient and staff encounters and interactions for communication quality improvement purposes.
Clinical Faculty
Center Staff
Stephanie Rosenberg
Systems Coordinator
617.638.1710
Stephanie.Rosenberg@bmc.org
Stephen Poole
Manager
617.638.1719
Kyle Weimer
Simulation Technician
William Platt
Simulation Technician










