‘The Sky is the Limit’ for Who Could Benefit from BMC Brighton’s New Surgical Robot
|
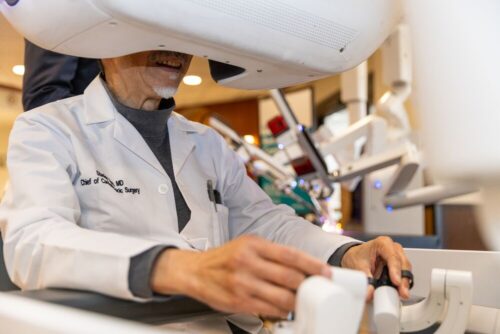
Michael O’Connor became a thoracic surgeon because he knew he wanted to join a dynamic and evolving field where he could treat people living with cancer. Advocating for his patients and his colleagues, he pushed for BMC Brighton to evolve as well, and helped the hospital upgrade its robotic surgery system to the “latest and greatest.”
The Latest Stories
Health equity news from Boston Medical Center
HealthCity is dedicated to sharing the most cutting-edge news and ideas for advancing health equity, both locally and nationally.